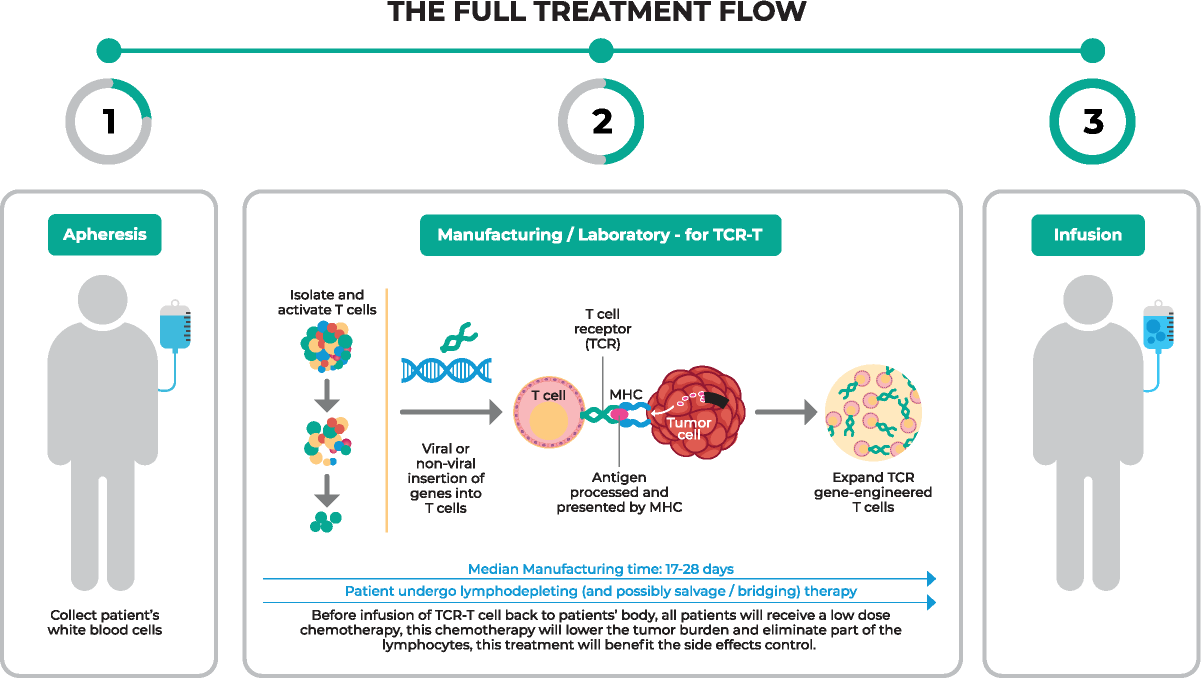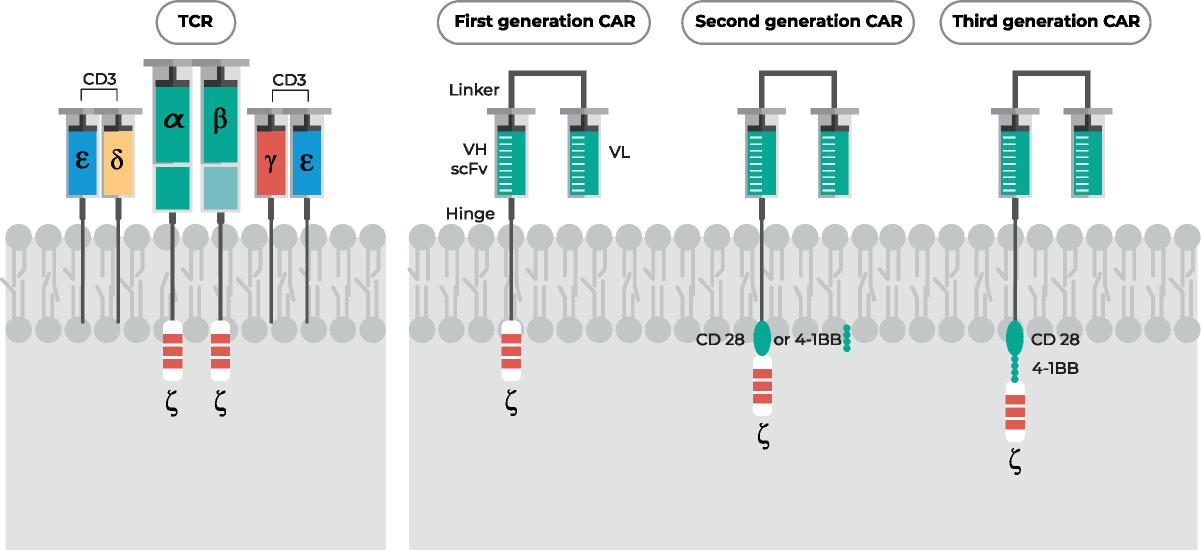
TCRs expressed on T cells can be genetically engineered in vitro to specifically recognize and kill cancer cells. Two approaches are used for TCR gene transfer. In the first approach, the antigen-specific TCR from PBMC- or TIL-derived cancer-specific T-cell clone is cloned, transduced into the peripheral blood T cells of patients using lentiviral or retroviral vectors, and subsequently amplified using the rapid expansion protocol. The second approach involves the generation of antigen-specific TCRs through the immunization of HLA-I/II transgenic mice with cancer antigen.
The antigen-specific TCR is cloned and transduced into the peripheral blood T cells of the patient for immunotherapy
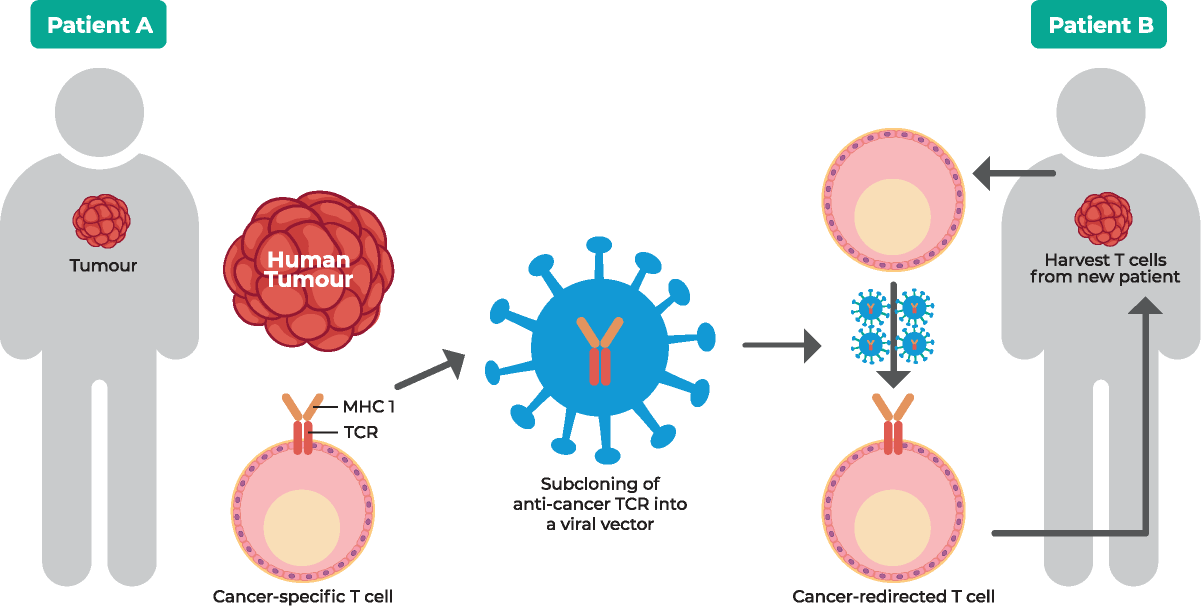
T-cell receptor (TCR)-engineered T cells for metastatic cancer treatment. Take the TCR genes from one patient who beat cancer and use them to engineer a cancer-fighting immune system in other patients.
(Source: https://researchoutreach.org/articles)Receiving the cancer signal – the T cell receptor58
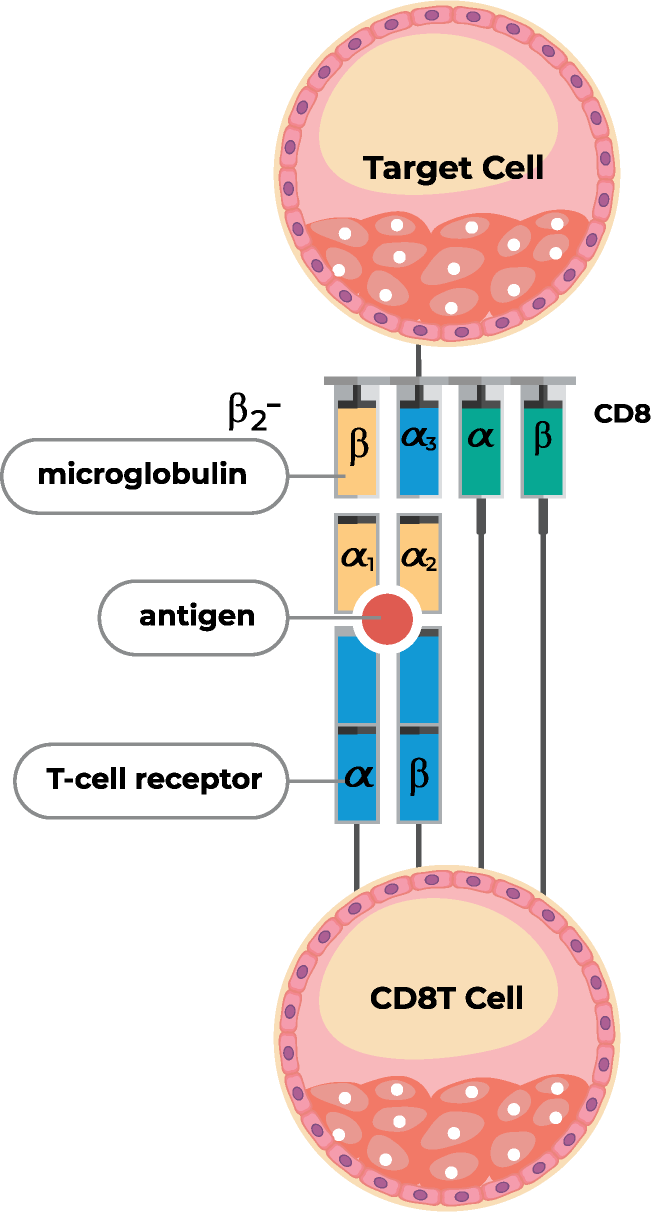
One class of white blood cells, known as T cells, has long been known to play an important role in the immune response to cancer. T cells harbor signaling proteins called T-cell receptors (TCR) on their surfaces, a feature that distinguishes them from other white blood cells. In a complex process, TCRs recognize pathogen- or tumor-specific proteins (known as antigens) that are presented by other immune cells and, also cancer cells.
Several T cell subsets exist, each with their own unique TCR and specialized function. Cytotoxic T cells and T helper (Th) cells are characterized by the presence of a CD8 or CD4 receptor on their cell surfaces, respectively. Cytotoxic T cells become activated when they recognize pathogens or tumor cells via their TCR. This is followed by the release of enzymes and toxic proteins that trigger programmed cell death in target cells. Th cells, as their name suggests, help other immune cells by releasing important chemical messengers called cytokines, which refine and regulate immune responses.